What is Periodontal Disease?
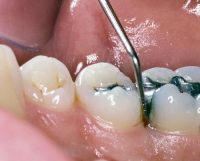
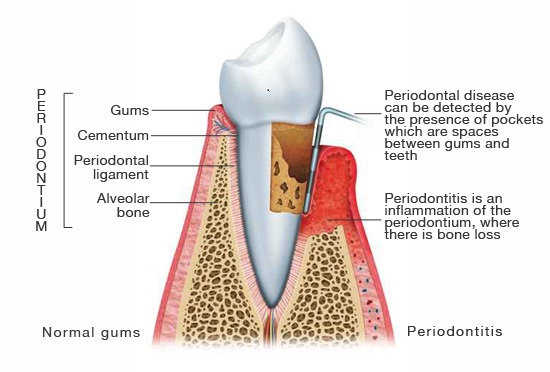
The word, “periodontal”, means “around the tooth”. A tooth does not attach directly to the bone. A healthy periodontal attachment consists of connective tissue fibers of the periodontal ligament, which connect the root of the tooth to the bone. These fibers also extend into the gum (gingiva), where the tooth emerges into the mouth. The gingiva then forms a tight cuff, or collar around the neck of the tooth.
Periodontitis:
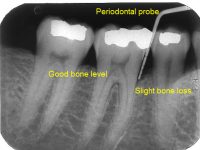
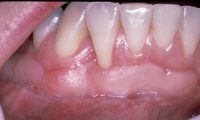
If undetected or untreated, inflammation in the gums (gingivitis) begins to extend deeper into the periodontal attachment. This inflammation causes detachment of the periodontal ligament from the tooth, and loss (resorption) of the supporting bone, resulting in periodontal pocket formation. Bacteria is then able to advance into the pocket, where it can no longer be removed by patient home care. Isolated from the oral environment, more aggressive bacteria begin to multiply, leading to infection and pus. Left untreated, pockets deepen, resulting in progressive bone loss and gum recession. Over time, teeth begin to loosen and shift, and are eventually lost. Periodontitis is the major cause of adult tooth loss.
Gingivitis:
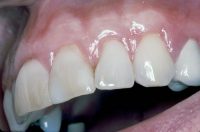
Bacterial plaque, which is present in all mouths, accumulates within the collar that the gum forms around the tooth. If the bacteria are not removed daily with effective brushing, flossing, or other appropriate techniques, the gums become inflamed. This condition is known as gingivitis, and it is characterized by sore, puffy gums, which bleed easily. Bad breath also results.
Even if you are brushing and flossing regularly, after a few months, some of the plaque will calcify around the teeth. This calcified plaque is known as tartar, or calculus, which can only be removed by a dentist or dental hygienist. The calculus has a rough, chalky surface, which harbors more bacterial plaque. When diagnosed at this early stage, the only treatment required is thorough professional scaling and polishing (prophylaxis), and effective home care by the patient.
Peri-Implant Disease:
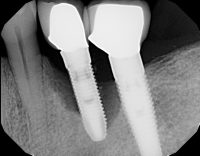
As more people have had teeth replaced with dental implants, we are seeing that gum inflammation and periodontal bone loss can affect dental implants as well as teeth! These conditions have been given the designations of “Peri-implant mucositis”, when soft tissues are involved, and “Peri-implantitis”, when bone loss has occurred around the implant. Although the bacterial and occlusal causes of peri-implant diseases are similar to those for periodontal diseases, their effect on implants is different.
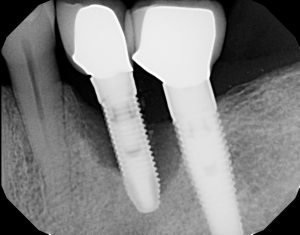
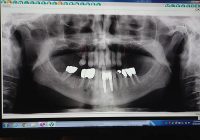
Advanced Bone loss middle implant
Since gum tissue does not actually attach to an implant in the same way it does to a tooth, when the gums become inflamed around an implant, they pull away from the implant more easily, and are often more tender than around teeth. Because implants connect directly to the bone, without an intervening periodontal ligament, implants do not gradually loosen, as teeth do, with progressive bone loss. Instead, implants tend to become very loose, all of a sudden, when the last bit of bone attachment is lost, and it’s too late to do anything about it.
Implants are more challenging to maintain after they have lost bone, because their textured, screw-shaped surfaces attract and retain plaque. They cannot be rendered smooth, like root planing can accomplish for a natural tooth, so implants present an intrinsic impediment to home plaque control and professional cleaning by the hygienist. At our office, we have specialized instrumentation, specifically designed for cleaning around dental implants, which have lost bone.
Occlusion and Periodontal Disease:
“Occlusion” refers to the bite relationships of your teeth when they come together. In a healthy mouth, all teeth come together evenly, and the jaws meet at a central position where teeth interlock comfortably. If one or more teeth contact before the others, or if contacts occur at an angle that pushes a tooth, this is known as an occlusal prematurity. Occlusal prematurities result in occlusal trauma to a tooth. Occlusal trauma by itself can cause an uncomfortable bite, bone loss around a dental implant, gum recession, and loosening of teeth. When superimposed on a tooth with periodontitis, occlusal trauma can increase bone loss around that tooth.
You will find no better medical team: all are capable and communicative, led by the highly skilled Dr. Pechter. All my questions were answered, everyone did their best to make me comfortable, including some lengthy procedures I needed. You can get a nice discount on certain services if you pay by check, always a nice option. This office gets my highest recommendation for consistently expert results.
A hearty and sincere thank you and well done! My teeth feel great due to your skills, diligence, thoroughness, and professionalism! Thank you very much.
Thank you for all your care and exceptional treatment over the past year. My dental implants have given me a beautiful smile and the confidence to eat whatever I desire.
I’ve been a patient of Dr. Stuart Pechter’s since 2001 and have been through numerous procedures in his well-run office. Every procedure has been pain-free and complication-free. Dr. Pechter truly has golden hands and superior expertise in the field of periodontics.
United States Marine Corps takes pleasure in recognizing Dr. Stuart Pechter for exemplary support and superior commitment. Your selfless dedication, level of commitment and assistance toward your Marine Recruiters is a testament to a heightened standard of excellence and is in keeping with the finest traditions of American patriotism and loyalty. Semper Fidelis!
Thank you for saving my teeth. I’m so glad I was referred to you for a second opinion. I wish I had come to you sooner. I never thought my teeth would ever feel this good again. Now I can really enjoy my wife’s cooking.
The Dental – Medical Connection
Several medical conditions are closely associated with periodontal disease. The most thoroughly researched of these is diabetes. It has been well established that diabetics have lowered resistance to bacterial infections in general, and to periodontitis in particular. Patients with either type I or type II diabetes will often display more severe inflammation of the gums and more rapid periodontal bone loss, which is often difficult to control. Newer research, however, indicates that the reverse is also true; the presence of periodontitis will worsen the severity of diabetes in these patients. It is especially important for patients with diabetes to be seeing a periodontist regularly. Not only are they at a higher risk for periodontal disease, but controlling their periodontal disease will improve control of their diabetes.
Periodontal disease has also been associated with other health issues, including heart disease and stroke. Researchers have found that people with periodontal disease are almost twice as likely to suffer from heart disease and have nearly twice the risk of a heart attack as those without periodontal disease. Current scientific findings have pointed to chronic inflammation around the teeth as the link between periodontal disease and other systemic inflammatory disorders, including cardiovascular disease, diabetes, rheumatoid arthritis, kidney disease, and even certain cancers. Although periodontitis may contribute to these medical conditions, this should not be interpreted to mean that periodontal disease has a causative role. More research is needed to pinpoint the precise biological mechanisms involved. However, since existing data has shown that patients with periodontal disease are at higher risk for these other medical conditions, it is important to consider periodontal health in any effort to achieve overall health. In the words of former Surgeon General C. Everett Koop, “A person is not healthy without good oral health.”
Pregnancy and Periodontal Disease:
A higher incidence of gum inflammation and periodontal involvement has long been observed in pregnant women. This condition has even been given the name of “pregnancy gingivitis”. It is thought to be related to hormonal changes which occur during pregnancy, that can lead to an exaggerated inflammatory response to oral bacteria. Since birth control pills work by mimicking the hormonal changes of pregnancy, women using oral contraceptives also show an increased incidence of periodontal involvement.
Recent research suggests that pregnant women with periodontal disease may be up to seven times more likely to have premature, underweight babies. The likely cause of this periodontitis – pregnancy problem is a labor-inducing chemical found in oral bacteria called prostaglandin. High levels of prostaglandin are found in women with severe periodontal disease. Other research has identified periodontal bacteria in the amniotic fluid of some pregnant women. Any disturbance to the amniotic fluid that surrounds the unborn baby, could be dangerous to both the mother and child.
If you are pregnant, or thinking of becoming pregnant, it is recommended that you have your teeth and gums checked for any signs of periodontal involvement as early as possible. If diagnosed, a non-surgical procedure known as scaling and root planing, may be recommended to remove bacteria and calculus (tartar) from the root surfaces of the teeth. If you are already pregnant, treatment would usually be performed during the second trimester of the pregnancy. Studies have shown that scaling and root planing may reduce the risk of preterm, low birth weight babies for pregnant women with periodontal disease by up to 84%.
Customer Feedback
You will find no better medical team: all are capable and communicative, led by the highly skilled Dr. Pechter. All my questions were answered, everyone did their best to make me comfortable, including some lengthy procedures I needed. You can get a nice discount on certain services if you pay by check, always a nice option. This office gets my highest recommendation for consistently expert results.
A hearty and sincere thank you and well done! My teeth feel great due to your skills, diligence, thoroughness, and professionalism! Thank you very much.
Thank you for all your care and exceptional treatment over the past year. My dental implants have given me a beautiful smile and the confidence to eat whatever I desire.
I’ve been a patient of Dr. Stuart Pechter’s since 2001 and have been through numerous procedures in his well-run office. Every procedure has been pain-free and complication-free. Dr. Pechter truly has golden hands and superior expertise in the field of periodontics.
United States Marine Corps takes pleasure in recognizing Dr. Stuart Pechter for exemplary support and superior commitment. Your selfless dedication, level of commitment and assistance toward your Marine Recruiters is a testament to a heightened standard of excellence and is in keeping with the finest traditions of American patriotism and loyalty. Semper Fidelis!
Thank you for saving my teeth. I’m so glad I was referred to you for a second opinion. I wish I had come to you sooner. I never thought my teeth would ever feel this good again. Now I can really enjoy my wife’s cooking.

Stuart B. Pechter, D.M.D.
1280 Lantana Rd
Lantana, FL 33462
Phone: (561) 582-5207
Email: info@pechterperio.com